The testicles are the two egg-shaped male sex glands suspended in the scrotal sac behind the penis. They normally develop inside the abdominal cavity and then descend through the inguinal canal into the scrotum shortly before birth or during the first few months of life. In about 3 percent of full term and 30 percent of premature baby boys, however, one or both testicles fail to fully descend, a condition known medically as cryptorchidism There are varying degrees of the condition. With true cryptorchidism, a testicle is not visible nor can it be felt when the baby is in a supine, frog legged position. The condition is due usually to mechanical or hormonal abnormalities. Maldescent, incomplete testicular descent, or arrested testis refers to a testicle that has descended only partially to the scrotum, the result of mechanical barriers to complete passage When certain conditions cause a testicle to move off the normal course of descent and settle elsewhere, such as along the inner thigh or above the pubic bone, this is referred to as an ectopic or misplaced testis. In cases of highly mobile or retractile testes, a testicle is positioned properly in the scrotum only at certain times at other times it retracts up into the inguinal canal or abdomen, due to tightening and squeezing of the muscle that lines the scrotum. This usually harmless condition, sometimes called pseudocryptorchidism, eventually abates, leaving normal genital structure and sexual function. During a thorough examination of the baby in a warm tub it is possible to differentiate between a truly undescended and a retractile testicle. Although some types of undescended testicles have no impact on sexual function or fertility, true cryptorchidism may result in a poorly developed testicle that cannot produce viable sperm. When both testicles are so affected, the condition results in sterility if left untreated. Men with a problem in testicular descent have an increased incidence of testicular cancer, and therefore should be particularly careful about regularly doing self examination of their testes and having medical checkups.
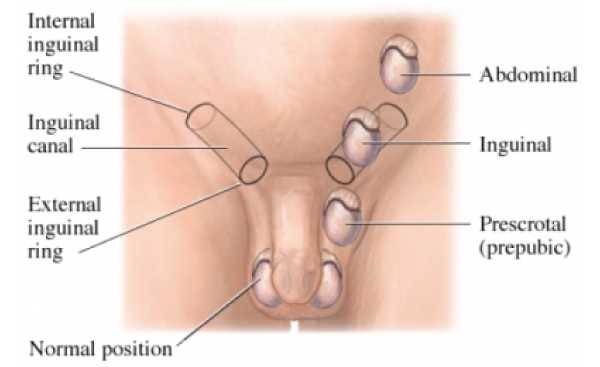
Diagnostic Studies And Procedures
Parents are likely to suspect an undescended testicle if the baby’s scrotum is totally flat or flat on one side. A physical examination by the pediatrician can confirm the diagnosis. Depending on the nature of the problem, other tests may be ordered, including ultrasound and other imaging studies and hormonal and genetic evaluations.
Medical Treatments
No treatment is advised for retractile testes as a rule, because they rarely cause problems and tend to become normal by puberty. Otherwise, treatment will depend on the type of cryptorchidism and the doctor’s approach. In many instances, the recommendation will be to wait and see what happens, because about 80 percent of misplaced testes descend normally within the first year of life. In some cases of true cryptorchidism, doctors will prescribe intramuscular injections of the hormone human chorionic gonadotropin , to be given several times a week for five weeks. Such hormonal therapy may promote normal testicular descent. When hormonal treatment fails, surgery may be recommended. In one surgical approach, orchiopexy, the undescended testicle is repositioned into the scrotum. This is usually done before two years of age because any delay, especially beyond the age of five, may impair the boy’s normal sperm production. If an abnormal testicle has not corrected itself by puberty, then removing it may be advised. An artificial implant can be placed in the scrotum so that the testicles appear normal. The decision to do so can be particularly important psychologically. In the rare cases in which both testicles must be removed, the boy will be given injections of male sex hormones at puberty to ensure normal growth and development. Hormonal therapy will continue for life, making normal sexual function possible, even though the man will be infertile.
Alternative Therapies
No alternative therapy can aid promote descent of the testicles.
Self Treatment
Parents should never try to reposition a baby’s testicle manually; such maneuvering could cause serious damage. A boy who has had a testicular descent problem should be taught the techniques of testicular self examination at puberty and instructed to perform the simple, three minute check once a month throughout life . Starting young is important because it may take several months for the boy to get to know his own body. Any abnormality in sexual development can cause serious psychological problems. In those unusual cases in which sterility occurs, it is important that parents assure their son that he is normal in other respects, and that with proper hormone therapy, he can also function sexually, even though he will not be able to father children.
Other Causes of Absent or Abnormal Testicles
Various hormonal and genetic disorders can result in a baby with absent or incomplete sex organs, but these syndromes are very rare.